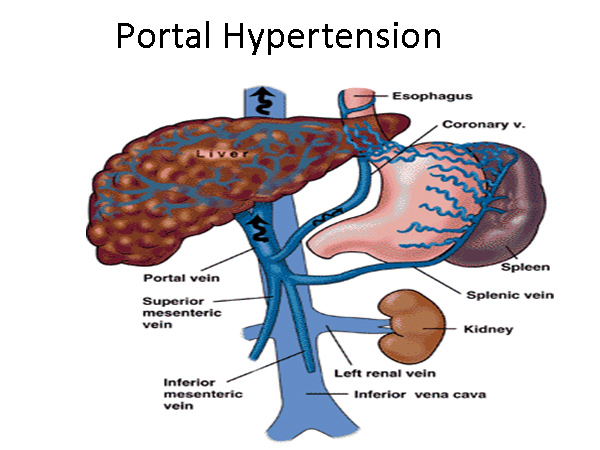
Definition of portal hypertension:
A potential complication of chronic alcoholism resulting in liver damage and obstruction of venous blood flow through the liver. The rising blood pressure in the veins between the gastrointestinal tract and liver causes engorgement of veins around the umbilicus (navel). The characteristic radiating pattern of veins is called a “caput medusae” (head of Medusa). Medusa was the “snake-haired lady” in Greek mythology.
Signs and symptoms of Portal Hypertension
The onset of portal hypertension may not always be associated with specific symptoms that identify what is happening in the liver. But if you have liver disease that leads to cirrhosis, the chance of developing portal hypertension is high.
The main symptoms and complications of portal hypertension include:
The main symptoms and complications of portal hypertension include:
- Gastrointestinal bleeding marked by black, tarry stools or blood in the stools, or vomiting of blood due to the spontaneous rupture and hemorrhage from varices
- Ascites (an accumulation of fluid in the abdomen)
- Encephalopathy or confusion and forgetfulness caused by poor liver function
- Reduced levels of platelets, blood cells that help form blood clots, or white blood cells, the cells that fight infection
Causes and Risk Factors
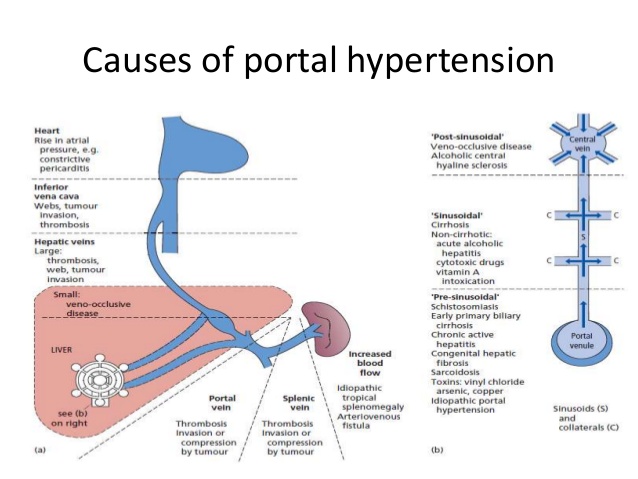
The most common cause of portal hypertension is cirrhosis of the liver.Cirrhosis is scarring which accompanies the healing of liver injury caused by hepatitis, alcohol, or other less common causes of liver damage. In cirrhosis, the scar tissue blocks the flow of blood through the liver.
Other causes of portal hypertension include blood clots in the portal vein, blockages of the veins that carry the blood from the liver to theheart, a parasitic infection called schistosomiasis, and focal nodular hyperplasia, a disease seen in people infected with HIV, the virus that may lead to AIDS. Sometimes the cause is unknown.
Other causes of portal hypertension include blood clots in the portal vein, blockages of the veins that carry the blood from the liver to theheart, a parasitic infection called schistosomiasis, and focal nodular hyperplasia, a disease seen in people infected with HIV, the virus that may lead to AIDS. Sometimes the cause is unknown.
Diagnosis
Usually, doctors make the diagnosis of portal hypertension based on the presence of ascites or of dilated veins or varices as seen during a physical exam of the abdomen or the anus. Various lab tests, X-ray tests, and endoscopic exams may also be used.
Treatment
Unfortunately, most causes of portal hypertension cannot be treated. Instead, treatment focuses on preventing or managing the complications, especially the bleeding from the varices. Diet,medications, endoscopic therapy, surgery, and radiology procedures all have a role in treating or preventing the complications. Other treatment depends on the severity of the symptoms and on how well your liver is functioning.
Treatment may include:
Other Treatment Options for Portal Hypertension
If endoscopic therapy, drug therapy, and/or dietary changes don't successfully control variceal bleeding, you may require one of the following procedures to reduce the pressure in these veins. Decompression procedures include:
Treatment may include:
- Endoscopic therapy. This is usually the first line of treatment for variceal bleeding and consists of either banding or sclerotherapy. Banding is a procedure in which a gastroenterologist uses rubber bands to block off the blood vessel to stop bleeding. Sclerotherapy is occasionally used when banding cannot be used and is a procedure in which a blood-clotting solution is injected into the bleeding varices to stop bleeding.
- Medications. Nonselective beta-blockers (nadolol orpropranolol) may be prescribed alone or in combination with endoscopic therapy to reduce the pressure in varices and further reduce the risk of bleeding. Nonselective beta blockers are also prescribed to prevent a first variceal hemorrhage in a patient with varices that are felt to be at risk for bleeding. Esophageal variceal banding has also been used for that purpose, especially in patients who can't take beta blockers. The drug lactulose can help treat confusion and other mental changes associated with encephalopathy.
Other Treatment Options for Portal Hypertension
If endoscopic therapy, drug therapy, and/or dietary changes don't successfully control variceal bleeding, you may require one of the following procedures to reduce the pressure in these veins. Decompression procedures include:
- Transjugular intrahepatic portosystemic shunt (TIPS): This procedure involves placing astent (a tubular device) in the middle of the liver. The stent connects the hepatic vein with the portal vein, which reroutes blood flow in the liver and helps relieve pressure in abnormal veins.
- Distal splenorenal shunt (DSRS):This procedure connects the vein from your spleen to the vein from the left kidney in order to reduce pressure in the varices and control bleeding.
What Lifestyle Changes Should Be Made for Portal Hypertension?
Maintaining good nutritional habits and keeping a healthy lifestyle may help you avoid portal hypertension. Some of the things you can do to improve the function of your liver include the following:
- Do not use alcohol or street drugs.
- Do not take any over-the-counter or prescription drugs or herbal medicines without first consulting your doctor or nurse. (Some medications may make liver disease worse.)
- Follow the dietary guidelines given by your health care provider, including eating a low-sodium (salt) diet. You will probably be required to consume no more than 2 grams of sodium per day. Reduced protein intake may be required if confusion is a symptom. A dietitian can create a meal plan for you.