Definition
|
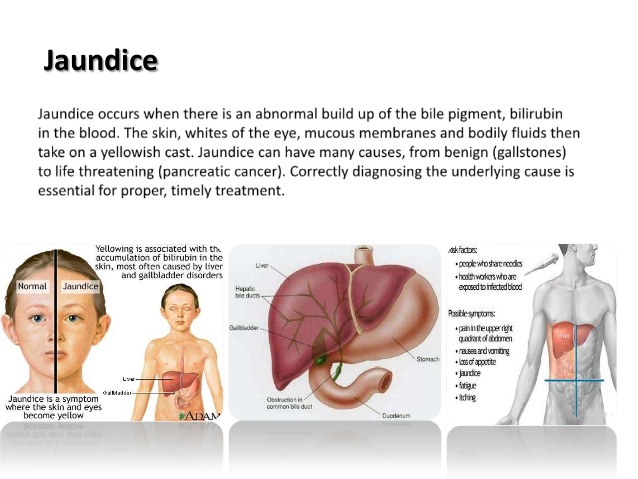
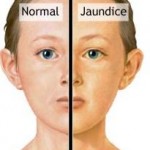
Jaundice literally means “yellow” in French. Yellowing of the skin and whites of the eyes from a backup of bile metabolic by-products from the blood into body tissues. May result from blockage of the ducts draining bile from the liver into the intestines or excessive breakdown of red blood cells. Hemoglobin from destroyed RBCs is broken down, and in part, ends up in bile secretions.
|
Signs and symptoms
Yellow-tinted skin and eyes characterize jaundice. In more severe cases, the whites of your eyes may turn brown or orang-colored. You may also have dark urine and pale stools. If an underlying health condition such as viral hepatitis is to blame for the jaundice, you might experience other symptoms, such as excessive fatigue and vomiting.
Causes of Jaundice
Old red blood cells travel to your liver, where they’re broken down. Bilirubin is the yellow pigment formed by the breakdown of these old cells. Jaundice occurs when your liver doesn’t metabolize bilirubin the way it’s supposed to.
Your liver might be damaged and unable to perform this process. Sometimes, the bilirubin simply can’t make it to your digestive tract, where it normally would be removed through your stool. In other cases, there may be too much bilirubin trying to enter the liver at once, or too many red blood cells dying at one time.
Jaundice in adults is often indicative of:
Your liver might be damaged and unable to perform this process. Sometimes, the bilirubin simply can’t make it to your digestive tract, where it normally would be removed through your stool. In other cases, there may be too much bilirubin trying to enter the liver at once, or too many red blood cells dying at one time.
Jaundice in adults is often indicative of:
- alcohol abuse
- liver infection
- liver cancer
- cirrhosis (scarring of the liver, usually due to alcohol)
- gallstones (cholesterol stones made of hardened fat material or pigment stones made of bilirubin)
- hepatitis (swelling of the liver that decreases its ability to function)
- pancreatic cancer
- parasites in the liver
- blood disorders, such as hemolytic anemia (a decreased amount of red blood cells in the body, which leads to fatigue and weakness)
- an adverse reaction to or overdose of a medication, such as acetaminophen
Diagnosis
Your doctor will first conduct blood tests to determine the cause of your jaundice. A blood test can not only determine the total amount of bilirubin in your body, but it can also help detect indicators of other diseases such as hepatitis.
Other diagnostic tests may be used, including:
Other diagnostic tests may be used, including:
- liver function tests: a series of blood tests that measure levels of certain proteins and enzymes the liver produces when it’s healthy and when it’s damaged
- imaging studies: includes abdominal ultrasounds (using high-frequency sound waves to generate images of your internal organs), computed tomography (CT) scan, and/or magnetic resonance imaging (MRI) tests
- liver biopsies: small samples of liver tissue are removed for testing and microscopic examination
Treatment
The type of treatment your doctor recommends for jaundice depends on the underlying cause. Mild cases may go away without treatment. However, severe cases can eventually damage the brain. Your doctor will treat the cause of the jaundice, not the symptom itself. Once treatment begins, your yellow skin will likely diminish.
According to the American Liver Foundation, most jaundice cases in infants resolve within one to two weeks.
Moderate jaundice is typically treated with phototherapy (light therapy) in the hospital or in the home to help remove excess bilirubin.
The light waves used in phototherapy are absorbed by your baby’s skin and blood. The light helps your baby’s body change the bilirubin into waste products to be eliminated. Frequent bowel movements with greenish stools are a common side effect of this therapy. This is just the bilirubin exiting the body. Phototherapy may involve the use of a lighted pad, which mimics natural sunlight and is placed on your baby’s skin.
Severe cases of jaundice are treated with blood transfusions (injections of donor blood) to remove bilirubin.
According to the American Liver Foundation, most jaundice cases in infants resolve within one to two weeks.
Moderate jaundice is typically treated with phototherapy (light therapy) in the hospital or in the home to help remove excess bilirubin.
The light waves used in phototherapy are absorbed by your baby’s skin and blood. The light helps your baby’s body change the bilirubin into waste products to be eliminated. Frequent bowel movements with greenish stools are a common side effect of this therapy. This is just the bilirubin exiting the body. Phototherapy may involve the use of a lighted pad, which mimics natural sunlight and is placed on your baby’s skin.
Severe cases of jaundice are treated with blood transfusions (injections of donor blood) to remove bilirubin.
Conditions of Jaundice
1. Conditions Related with the Red Blood Cells
An increase in the rate of breakdown of the red blood cells usually results in increased bilirubin production, which may circulate in the bloodstream. Liver cells are not able to keep up with the pace to process excess bilirubin, resulting in build-up and spillage in the blood. Conditions that lead to an increased red blood cell breakdown include:
2. Conditions Related with the Liver Cells
Conditions involving your liver cells may cause build-up of excess bilirubin. You may have a liver enzyme deficiency, an obstruction to the flow of bilirubin from the liver to the bile ducts, or a problem with damaged liver cells. These conditions may result in poor processing of bilirubin, which may spill into the bloodstream to cause jaundice. Liver cell problems that may cause abnormal bilirubin production include:
3. Conditions Related with the Tiny Bile Ducts
The liver has small bile ducts that allow passage of bile, containing bilirubin, for excretion. If these bile ducts are narrowed or damaged, bile flow becomes restricted. Bile spills into your bloodstream, leading to jaundice. Primary biliary cirrhosis and primary sclerosing cholangitis are examples of bile duct problems.
4. Conditions Related with the Common Bile Duct
From the bile ducts, bilirubin-containing bile drains from the liver into your common bile duct (CBD). Obstruction of the CBD causes excess bile to join the bloodstream, leading to jaundice. Conditions that cause obstructive jaundice include:
- Genetic conditions such as thalassemia, sickle cell anemia, G6-PD deficiency, and spherocytosis
- Malaria
- Hemolytic uremic syndrome
2. Conditions Related with the Liver Cells
Conditions involving your liver cells may cause build-up of excess bilirubin. You may have a liver enzyme deficiency, an obstruction to the flow of bilirubin from the liver to the bile ducts, or a problem with damaged liver cells. These conditions may result in poor processing of bilirubin, which may spill into the bloodstream to cause jaundice. Liver cell problems that may cause abnormal bilirubin production include:
- Hepatitis or liver inflammation, which may be caused by an infection, alcohol abuse, autoimmune disorder, poisoning, or a side-effect of certain medications.
- Cirrhosis or scarring of the liver (fibrosis), which is a slow, progressive condition that does not cause early symptoms, but leads to jaundice when liver function is severely affected.
- Rare hereditary defects in liver enzymes involved in processing bilirubin, such as Gilbert's syndrome, Crigler-Najjar syndrome, Rotor's syndrome, and Dubin-Johnson syndrome.
3. Conditions Related with the Tiny Bile Ducts
The liver has small bile ducts that allow passage of bile, containing bilirubin, for excretion. If these bile ducts are narrowed or damaged, bile flow becomes restricted. Bile spills into your bloodstream, leading to jaundice. Primary biliary cirrhosis and primary sclerosing cholangitis are examples of bile duct problems.
4. Conditions Related with the Common Bile Duct
From the bile ducts, bilirubin-containing bile drains from the liver into your common bile duct (CBD). Obstruction of the CBD causes excess bile to join the bloodstream, leading to jaundice. Conditions that cause obstructive jaundice include:
- Gallstone formation, which may occur in the gallbladder, but gallstone get stuck in the CBD
- Cancer in the pancreas
- Pancreatitis, or inflammation of the pancreas, causing swelling of the organ
- Biliary atresia, a condition where inflamed bile ducts become fibrotic (scarred)
- Gallbladder cancer
Causes of Jaundice in Pregnancy
Cholestasis of pregnancy. This uncommon condition, which occurs during the last trimester, usually affects women from Chile and Scandinavia, and tends to occur with every pregnancy. It is also associated with the use of oral estrogens. Women with this condition experience severe itchiness and may have an increased risk of developing gallstones. Fetal developmental abnormalities are also possible.
Pre-Eclampsia. This condition is characterized by high blood pressure, increased fluid retention, anemia, and kidney damage. Destruction of red blood cells increases bilirubin levels, but jaundice is not common.
Acute fatty liver of pregnancy. This is a very serious complication associated with pre-eclampsia. It results in liver failure, but delivery of the fetus may reverse it. Jaundice may occur, but not in all patients. Infant death is also a possible risk.
Prevention of Jaundice
Jaundice may be prevented by avoiding the underlying cause. These include:
Pre-Eclampsia. This condition is characterized by high blood pressure, increased fluid retention, anemia, and kidney damage. Destruction of red blood cells increases bilirubin levels, but jaundice is not common.
Acute fatty liver of pregnancy. This is a very serious complication associated with pre-eclampsia. It results in liver failure, but delivery of the fetus may reverse it. Jaundice may occur, but not in all patients. Infant death is also a possible risk.
Prevention of Jaundice
Jaundice may be prevented by avoiding the underlying cause. These include:
- Avoiding heavy use of alcohol use to prevent alcoholic hepatitis, pancreatitis, or cirrhosis
- Getting vaccinations for hepatitis A and hepatitis B
- Taking medications to prevent malaria before traveling to high-risk areas
- Avoiding high-risk behaviors (drug abuse or unprotected sex, which can cause hepatitis B)
- Avoiding potentially contaminated water or food, and maintaining good hygiene to prevent hepatitis A
- Avoiding toxic medications or substances that may cause hemolysis (breakdown of red blood cells) or liver damage.