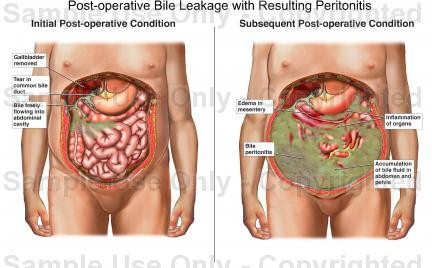
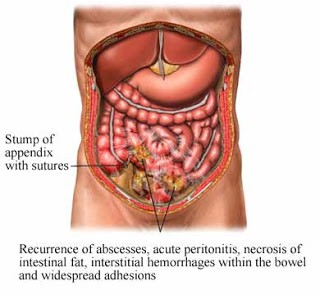
Definition of peritonitis
Peritonitis is inflammation of the peritoneum. The inflammation is usually the result of a fungal or bacterial infection caused by an abdominal injury, an underlying medical condition, or a treatment device, such as a dialysis catheter or feeding tube. Before antibiotics, people would die from peritonitis if an inflamed appendix burst. Indications of peritonitis are called “peritoneal signs”: tender abdomen, rebound pain (pain when manual pressure released from examining abdomen), board-like rigidity of abdominal muscles, no bowel sounds (gurgles). The peritoneal membrane is very sensitive to exposure to foreign substances. Contact with blood, bile, urine, pus will cause peritoneal signs. Peritonitis is a serious condition that needs immediate medical attention. Prompt intravenous antibiotics are needed to treat the infection. Surgery is sometimes necessary to remove infected tissue. The infection can spread and become life-threatening if it isn’t treated promptly.
Signs and symptoms of peritonitis The first symptoms of peritonitis are typically poor appetite and nausea and a dull abdominal ache that quickly turns into persistent, severe abdominal pain, which is worsened by any movement.
Other signs and symptoms related to peritonitis may include:
Risk Factors
Factors that increase your risk of peritonitis include:
Causes of peritonitis
The two main types of peritonitis are primary spontaneous peritonitis, an infection that develops in the peritoneum; and secondary peritonitis, which usually develops when an injury or infection in the abdominal cavity allows infectious organisms into the peritoneum. Both types of peritonitis are life-threatening. The death rate from peritonitis depends on many factors, but can be as high as 40% in those who also have cirrhosis. As many as 10% may die from secondary peritonitis.
Peritonitis is inflammation of the peritoneum. The inflammation is usually the result of a fungal or bacterial infection caused by an abdominal injury, an underlying medical condition, or a treatment device, such as a dialysis catheter or feeding tube. Before antibiotics, people would die from peritonitis if an inflamed appendix burst. Indications of peritonitis are called “peritoneal signs”: tender abdomen, rebound pain (pain when manual pressure released from examining abdomen), board-like rigidity of abdominal muscles, no bowel sounds (gurgles). The peritoneal membrane is very sensitive to exposure to foreign substances. Contact with blood, bile, urine, pus will cause peritoneal signs. Peritonitis is a serious condition that needs immediate medical attention. Prompt intravenous antibiotics are needed to treat the infection. Surgery is sometimes necessary to remove infected tissue. The infection can spread and become life-threatening if it isn’t treated promptly.
Signs and symptoms of peritonitis The first symptoms of peritonitis are typically poor appetite and nausea and a dull abdominal ache that quickly turns into persistent, severe abdominal pain, which is worsened by any movement.
Other signs and symptoms related to peritonitis may include:
- Abdominal tenderness or distention
- Chills
- Fever
- Fluid in the abdomen
- Extreme thirst
- Not passing any urine, or passing significantly less urine than usual
- Difficulty passing gas or having a bowel movement
- Vomiting
Risk Factors
Factors that increase your risk of peritonitis include:
- Peritoneal dialysis. Peritonitis is common among people undergoing peritoneal dialysis therapy.
- Other medical conditions. The following medical conditions increase your risk of developing peritonitis: cirrhosis, appendicitis, Crohn's disease, stomach ulcers, diverticulitis and pancreatitis.
- History of peritonitis. Once you've had peritonitis, your risk of developing it again is higher than it is for someone who has never had peritonitis.
Causes of peritonitis
The two main types of peritonitis are primary spontaneous peritonitis, an infection that develops in the peritoneum; and secondary peritonitis, which usually develops when an injury or infection in the abdominal cavity allows infectious organisms into the peritoneum. Both types of peritonitis are life-threatening. The death rate from peritonitis depends on many factors, but can be as high as 40% in those who also have cirrhosis. As many as 10% may die from secondary peritonitis.
The most common risk factors for primary spontaneous peritonitis include:
Diagnosis of Peritonitis
If you have any symptoms of peritonitis, call your doctor right away. Seeking prompt medical attention is especially important for peritoneal dialysis patients who have a combination of abdominal pain and a clouding of the peritoneal fluid, which is caused by a build up of infection-fighting white blood cells.
Because peritonitis can rapidly lead to potentially fatal complications such as sepsis and septic shock, which causes a massive drop in blood pressure, organ failure, and death, it’s essential to receive a quick diagnosis followed by appropriate treatment.
Your doctor will ask about your symptoms and medical history, and conduct a thorough physical examination, including assessment of tension and tenderness in the abdomen.
Diagnostic tests for peritonitis may include:
Treatments for Peritonitis
If you're diagnosed with peritonitis, you'll be admitted to a hospital. Typically, you'll immediately start receiving intravenous antibiotics or antifungal medications to treat the infection. Additional supportive treatments will be necessary if organ failure from sepsis develops as a complication of the infection. Such treatments may include intravenous fluids, drugs to maintain blood pressure, and nutritional support.
If you have peritoneal dialysis-associated peritonitis, you may receive medications that are injected directly into the peritoneal tissue, a strategy that some studies have reported to be more effective than intravenous medications. Until the peritonitis is cured, you will need to use another method of dialysis, such as hemodialysis.
In many cases, emergency surgery is required, especially if peritonitis has been caused by conditions such as appendicitis, a perforated stomach ulcer, or diverticulitis. Infected tissue such as a burst appendix or abscess will be surgically removed. So will any part of the peritoneal tissue that has been seriously damaged by infection.
During your hospitalization, you will be closely monitored for signs of sepsis and septic shock, which usually require immediate transfer to an intensive care unit.
Preventing Peritonitis
Although peritonitis can be a complication of peritoneal dialysis, it's much less common than it used to be because of improved technology and self-care techniques that are taught during initial training.
If you're receiving peritoneal dialysis, you can lower your risk of peritonitis by following these tips:
- Liver disease with cirrhosis . Such disease often causes a buildup of abdominal fluid (ascites) that can become infected.
- Kidney failure getting peritoneal dialysis. This technique, which involves the implantation of a catheter into the peritoneum, is used to remove waste products in the blood of people with kidney failure. It's linked to a higher risk of peritonitis due to accidental contamination of the peritoneum by way of the catheter.
- an abdominal wound or injury
- a ruptured appendix
- a stomach ulcer
- a perforated colon
- diverticulitis, which is when pouches form on the wall of the colon and become inflamed
- pancreatitis, which is an inflammation of the pancreas
- cirrhosis of the liver or other types of liver disease
- infection of the gallbladder, intestines, or bloodstream
- pelvic inflammatory disease, which is an infection of a woman’s reproductive organs
- Crohn’s disease, which is a type of inflammatory bowel disease
- invasive medical procedures, including treatment for kidney failure, surgery, or the use of a feeding tube
Diagnosis of Peritonitis
If you have any symptoms of peritonitis, call your doctor right away. Seeking prompt medical attention is especially important for peritoneal dialysis patients who have a combination of abdominal pain and a clouding of the peritoneal fluid, which is caused by a build up of infection-fighting white blood cells.
Because peritonitis can rapidly lead to potentially fatal complications such as sepsis and septic shock, which causes a massive drop in blood pressure, organ failure, and death, it’s essential to receive a quick diagnosis followed by appropriate treatment.
Your doctor will ask about your symptoms and medical history, and conduct a thorough physical examination, including assessment of tension and tenderness in the abdomen.
Diagnostic tests for peritonitis may include:
- Blood and urine tests
- Imaging studies such as X-rays and computerized tomography (CT) scans
- Exploratory surgery
Treatments for Peritonitis
If you're diagnosed with peritonitis, you'll be admitted to a hospital. Typically, you'll immediately start receiving intravenous antibiotics or antifungal medications to treat the infection. Additional supportive treatments will be necessary if organ failure from sepsis develops as a complication of the infection. Such treatments may include intravenous fluids, drugs to maintain blood pressure, and nutritional support.
If you have peritoneal dialysis-associated peritonitis, you may receive medications that are injected directly into the peritoneal tissue, a strategy that some studies have reported to be more effective than intravenous medications. Until the peritonitis is cured, you will need to use another method of dialysis, such as hemodialysis.
In many cases, emergency surgery is required, especially if peritonitis has been caused by conditions such as appendicitis, a perforated stomach ulcer, or diverticulitis. Infected tissue such as a burst appendix or abscess will be surgically removed. So will any part of the peritoneal tissue that has been seriously damaged by infection.
During your hospitalization, you will be closely monitored for signs of sepsis and septic shock, which usually require immediate transfer to an intensive care unit.
Preventing Peritonitis
Although peritonitis can be a complication of peritoneal dialysis, it's much less common than it used to be because of improved technology and self-care techniques that are taught during initial training.
If you're receiving peritoneal dialysis, you can lower your risk of peritonitis by following these tips:
- Thoroughly wash your hands, including the areas between your fingers and under your fingernails, before touching the catheter.
- Wear a mouth/nose mask during exchanges.
- Observe the proper sterile exchange technique.
- Apply an antibiotic cream to the catheter exit site every day.