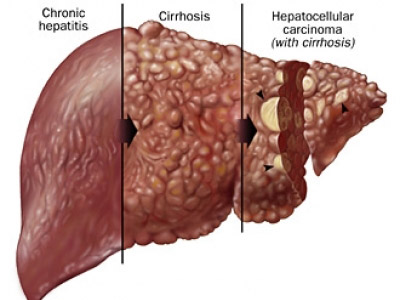
Definition of cirrhosis:
Literally, “orange-yellow” in Greek. A degenerative disease of the liver that often develops in chronic alcoholics, but can have other causes. The name refers to the gross appearance of the organ.
The liver weighs about 3 pounds and is the largest solid organ in the body. It performs many important functions, such as:
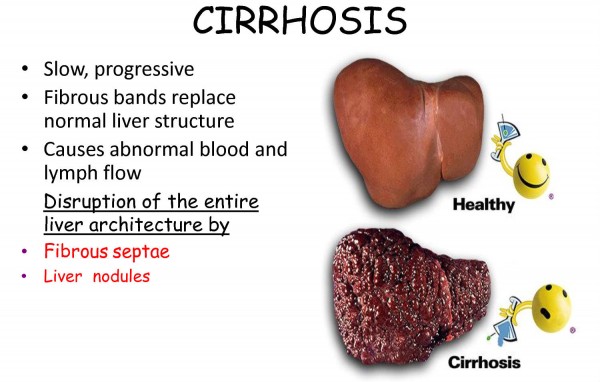
Cirrhosis is a slowly progressing disease in which healthy liver tissue is replaced with scar tissue, eventually preventing the liver from functioning properly. The scar tissue blocks the flow of blood through the liver and slows the processing of nutrients, hormones, drugs, and naturally produced toxins. It also slows the production of proteins and other substances made by the liver.
According to the National Institutes of Health, cirrhosis is the 12th leading cause of death by disease.
The liver weighs about 3 pounds and is the largest solid organ in the body. It performs many important functions, such as:
- Manufacturing blood proteins that aid in clotting, oxygen transport, and immune system function
- Storing excess nutrients and returning some of the nutrients to the bloodstream
- Manufacturing bile, a substance needed to help digest food
- Helping the body store sugar (glucose) in the form of glycogen
- Ridding the body of harmful substances in the bloodstream, including drugs and alcohol
- Breaking down saturated fat and producing cholesterol
Cirrhosis is a slowly progressing disease in which healthy liver tissue is replaced with scar tissue, eventually preventing the liver from functioning properly. The scar tissue blocks the flow of blood through the liver and slows the processing of nutrients, hormones, drugs, and naturally produced toxins. It also slows the production of proteins and other substances made by the liver.
According to the National Institutes of Health, cirrhosis is the 12th leading cause of death by disease.
Signs and symptoms of cirrhosis:
|
What Causes Cirrhosis of the Liver?
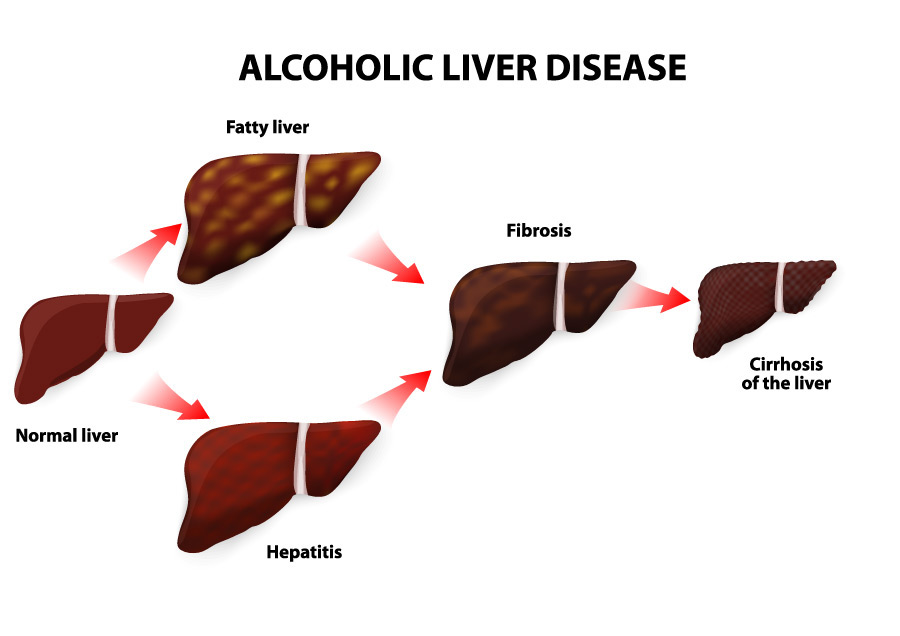
Hepatitis C, fatty liver, and alcohol abuse are the most common causes of cirrhosis of the liver in the U.S., but anything that damages the liver can cause cirrhosis, including:
- Fatty liver associated with obesity and diabetes
- Chronic viral infections of the liver (hepatitis types B, C, and D;Hepatitis D is extremely rare)
- Blockage of the bile duct, which carries bile formed in the liver to theintestines, where it helps in the digestion of fats; in babies, this can be caused by biliary atresia in which bile ducts are absent or damaged, causing bile to back up in the liver. In adults, bile ducts may become inflamed, blocked, or scarred, due to another liver disease called primary biliary cirrhosis.
- Repeated bouts of heart failure with fluid backing up into the liver
- Certain inherited diseases such as:
- Cystic fibrosis
- Glycogen storage diseases, in which the body is unable to process glycogen, a form of sugar that is converted to glucose and serves as a source of energy for the body
- Alpha 1 antitrypsin deficiency, an absence of a specific enzyme in the liver
- Diseases caused by abnormal liver function, such ashemochromatosis, a condition in which excessive iron is absorbed and deposited into the liver and other organs, and Wilson's disease, caused by the abnormal storage of copper in the liver
Diagnosis of Cirrhosis
People with early-stage cirrhosis of the liver usually don't have symptoms. Often, cirrhosis is first detected through a routine blood test or checkup. Your doctor may order one or more laboratory tests that may suggest a problem with your liver, such as cirrhosis.
Laboratory tests:
Laboratory tests:
- Liver function. Your blood is checked for excess bilirubin, which is a product of red blood cells breaking down, as well as for certain enzymes that may indicate liver damage.
- Kidney function. Your blood is checked for creatinine as kidney function may decline in later stages of cirrhosis (decompensated cirrhosis).
- Tests for hepatitis B and C. Your blood is checked for the hepatitis viruses.
- Clotting. Your international normalized ratio (INR) is checked for your blood's ability to clot.
- Magnetic resonance elastography or transient elastography. These noninvasive imaging tests detect hardening or stiffening of the liver and may eliminate the need for a liver biopsy.
- Other imaging tests. MRI, CT and ultrasound create images of the liver.
- Biopsy. A tissue sample (biopsy) is not necessarily needed to diagnose cirrhosis. However, your doctor may use it to identify the severity, extent and cause of liver damage.
Treatment for cirrhosis
Treatment for the underlying cause of cirrhosisIn early cirrhosis, it may be possible to minimize damage to the liver by treating the underlying cause. The options include:
Other medications can relieve certain symptoms, such as itching, fatigue and pain.
Nutritional supplements may be prescribed to counter malnutrition associated with cirrhosis and to prevent weak bones (osteoporosis).
Treatment for complications of cirrhosis:
Your doctor will work to treat any complications of cirrhosis, including:
Liver transplantation.
In advanced cases of cirrhosis, when the liver ceases to function, a liver transplant may be the only treatment option. People usually need to consider this option when they develop symptoms from cirrhosis, such as jaundice, significant fluid retention (ascites), bleeding varices, hepatic encephalopathy, kidney dysfunction, or liver cancer. A liver transplant replaces your liver with a healthy liver from a deceased donor or with part of a liver from a living donor. Cirrhosis is the most common reason for a liver transplant.
Candidates for liver transplant undergo extensive testing to determine whether they are healthy enough to have a good outcome following surgery. Additionally, transplant centers typically require some period of abstinence alcohol for people with alcohol-related liver disease before they can receive transplants.
Potential future treatments
Scientists are working to expand current treatments for cirrhosis, but success has been limited.
Because cirrhosis has numerous causes and complications, there are many potential avenues of approach. A combination of increased screening, lifestyle changes and new medications may improve outcomes for people with liver damage, if started early.
It may be possible in the future to decrease or even reverse the fibrosis that leads to cirrhosis depending on the cause of fibrosis. Some people who received successful hepatitis C treatment or hepatitis B medications may have improvement in their fibrosis.
Alternative medicine
A number of alternative medicines have been used to treat liver diseases. Milk thistle (silymarin) is the most widely used and best studied. Other herbs used include licorice root (glycyrrhiza), schisandra and astragalus. However, there is not enough evidence of benefit from clinical trials to recommend the use of any herbal products to treat liver cirrhosis. In addition, herbal medications represent an increasing percentage of reported cases of drug-induced liver injury. Talk with your doctor if you're interested in trying alternative medicine to help you cope with cirrhosis.
- Treatment for alcohol dependency. People with cirrhosis caused by alcohol abuse should stop drinking. If you have cirrhosis, it is essential to stop drinking since any amount of alcohol is toxic to the liver. If stopping alcohol use is difficult, your doctor may recommend a treatment program for alcohol addiction.
- Weight loss. People with cirrhosis caused by nonalcoholic fatty liver disease may become healthier if they lose weight and control their blood sugar levels. It is important to maintain adequate protein intake while attempting weight loss in the setting of cirrhosis.
- Medications to control hepatitis. Medications may limit further damage to liver cells caused by hepatitis B or C through specific treatment of these viruses.
- Medications to control other causes and symptoms of cirrhosis. Medications may slow the progression of certain types of liver cirrhosis. For example, for people with primary biliary cirrhosis (now known as primary biliary cholangitis) that is diagnosed early, medication may significantly delay progression to cirrhosis.
Other medications can relieve certain symptoms, such as itching, fatigue and pain.
Nutritional supplements may be prescribed to counter malnutrition associated with cirrhosis and to prevent weak bones (osteoporosis).
Treatment for complications of cirrhosis:
Your doctor will work to treat any complications of cirrhosis, including:
- Excess fluid in your body. A low-sodium diet and medication to prevent fluid buildup in the body may help control ascites and swelling. More-severe fluid buildup may require procedures to drain the fluid or other interventions to relieve pressure. At times, a small tube — a transjugular intrahepatic portosystemic shunt (TIPS) — is placed in the vein within the liver to reduce blood pressure in your liver and slow the rate of fluid accumulation.
- Portal hypertension. Certain blood pressure medications may control increased pressure in the veins that supply the liver (portal hypertension) and prevent severe bleeding. Your doctor will perform an upper endoscopy at regular intervals to look for enlarged veins in the esophagus or stomach (varices) that may bleed.
If you develop varices, you likely will need medication to reduce the risk of bleeding. If you are not able to tolerate medication and have signs that the varices are bleeding or are likely to bleed, you may need a procedure (band ligation) to stop the bleeding or reduce the risk of further bleeding. In severe cases, a TIPS can be placed in the vein within the liver to reduce blood pressure in your liver and to prevent further bleeding. - Infections. You may receive antibiotics or other treatments for infections. Your doctor also is likely to recommend vaccinations for influenza, pneumonia and hepatitis.
- Increased liver cancer risk. Your doctor will recommend blood tests and ultrasound exams every six months to look for signs of liver cancer.
- Hepatic encephalopathy. You may be prescribed medications to help prevent the buildup of toxins in your blood due to poor liver function.
Liver transplantation.
In advanced cases of cirrhosis, when the liver ceases to function, a liver transplant may be the only treatment option. People usually need to consider this option when they develop symptoms from cirrhosis, such as jaundice, significant fluid retention (ascites), bleeding varices, hepatic encephalopathy, kidney dysfunction, or liver cancer. A liver transplant replaces your liver with a healthy liver from a deceased donor or with part of a liver from a living donor. Cirrhosis is the most common reason for a liver transplant.
Candidates for liver transplant undergo extensive testing to determine whether they are healthy enough to have a good outcome following surgery. Additionally, transplant centers typically require some period of abstinence alcohol for people with alcohol-related liver disease before they can receive transplants.
Potential future treatments
Scientists are working to expand current treatments for cirrhosis, but success has been limited.
Because cirrhosis has numerous causes and complications, there are many potential avenues of approach. A combination of increased screening, lifestyle changes and new medications may improve outcomes for people with liver damage, if started early.
It may be possible in the future to decrease or even reverse the fibrosis that leads to cirrhosis depending on the cause of fibrosis. Some people who received successful hepatitis C treatment or hepatitis B medications may have improvement in their fibrosis.
Alternative medicine
A number of alternative medicines have been used to treat liver diseases. Milk thistle (silymarin) is the most widely used and best studied. Other herbs used include licorice root (glycyrrhiza), schisandra and astragalus. However, there is not enough evidence of benefit from clinical trials to recommend the use of any herbal products to treat liver cirrhosis. In addition, herbal medications represent an increasing percentage of reported cases of drug-induced liver injury. Talk with your doctor if you're interested in trying alternative medicine to help you cope with cirrhosis.
Facts about liver disease
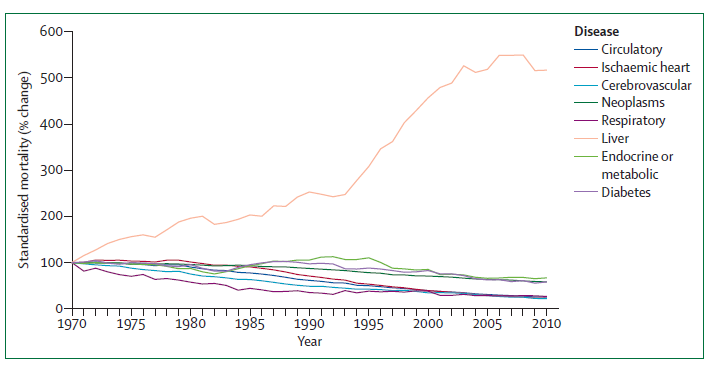
Comparative mortality rates
Graph: Data sourced from the Lancet Liver Campaign report: Addressing liver disease in the UK(Data were normalised to 100% in 1970, and subsequent trends plotted using the software Statistical Package for the Social Sciences. Data are from the WHO-HFA database.
- Analysed by Nick Sheron September, 2013).
Key facts
- Liver disease is the only major cause of death still increasing year-on-year
- Liver disease is the fifth ‘big killer’ in England & Wales, after heart, cancer, stroke and respiratory disease
- 16,087 people in the UK died from liver disease in 2008, a 4.5% increase since 2007.
- This includes 13,805 people in England and Wales, 1,903 in Scotland4 and 379 in Northern Ireland
- Twice as many people now die from liver disease as in 1991
- Liver disease kills more people than diabetes and road deaths combined.
These statistics are not comprehensive, due to two major reasons for under recording: the stigma associated with liver disease and attempts to avoid distress to the bereaved, and attribution of liver deaths to other codes as liver disease frequently causes multiple organ dysfunction.
It is important to remember that as people can survive with 70% liver damage, there is a substantial burden of morbidity from liver disease, a high cost to the NHS and a huge economic and human cost from liver-related ill health.
- Office for National Statisticshttps://www.ons.gov.uk/peoplepopulationandcommunity/birthsdeathsandmarriages/deaths
- British Liver Trust analysis of official mortality statistics covering all deaths related to liver dysfunction covering ICD K70-76 and other codes including C22-24 (liver cancer), and B15-B19 (viral hepatitis), December 2009.
- Office for National Statistics: Mortality Statistics, Deaths registered
- Public Health England liver profiles PHE Health Profiles – June 2015
- General Registrar Office for Scotland data on deaths: National Records of Scotland
- Northern Ireland Registrar General Annual Report 2008 – Section 6 Details – Causes of Death:http://www.nisra.gov.uk/
Alcohol and Liver Disease
- The cost to the NHS of alcohol misuse has been estimated at £2.7 billion each year. 1
- In 2007 4,580 people died in England and Wales from alcohol related liver disease. 2 There was a 41% increase in the number of deaths from alcohol related liver disease between 1999 and 2005 and in the last 30 years, mortality has risen over 450% in the UK. 3
- In 2007 in total, there were 5,732 alcohol-related deaths in men and 2,992 in women. 4
- The process is silent, but when liver disease has developed it presents as an acute illness with a 25-50% immediate mortality.
- Hospital admissions for alcohol related disease, including alcohol related liver disease, have more than doubled since 1995/6 and between 2002/3 and 2006/7 there was a 71% increase 5 .There are over 800,000 hospital admissions directly related and attributable to alcohol each year.6
- In Scotland, in 2007/8 there was a 400% increase in patients discharged from hospital with alcohol related liver disease (6,817) compared to 1996. 7 In 2006-7, 1,094 children aged under 18 were admitted to hospital with an alcohol-related diagnosis. Treatment for alcohol related conditions in Scotland costs over £1m a day.
- Department of Health: Safe, Sensible, Social – Consultation on further action Impact Assessments 22 July 2008
- ONS http://www.statistics.gov.uk/statbase/Product.asp?vlnk=14496
- Calling time: The nation’s drinking as a major health issue, Academy of Medical Sciences, 2004/The human cost of alcohol misuse BMA 2009
- ONS News release 27 01 09 http://www.statistics.gov.uk/cci/nugget.asp?id=1091
- North West Public Health Observatory (2008), ‘Local Alcohol Profiles for England’. Seehttp://www.nwph.net/alcohol/lape/
- CMO Annual Report Passive Drinking 2008 p.20 and Department of Health: Safe, Sensible, Social – Consultation on further action Impact Assessments 22 July 2008
- ISD SMR01, 11 June 2007
- The costs of alcohol use and misuse in Scotland, Scottish Government 2008